Discover the truth about chemical pregnancies and their impact on fertility.
Do chemical pregnancies make you more fertile?
Chemical pregnancies are a topic that often sparks curiosity and concern among couples trying to conceive. Understanding what a chemical pregnancy is, its impact on fertility, and how to cope with it is crucial for those who have experienced this early pregnancy loss. In this article, we will explore the science behind chemical pregnancies, their effects on fertility, and the emotional aspects of coping with such a loss. We will also discuss prevention strategies and planning for future pregnancies after experiencing a chemical pregnancy.
Understanding Chemical Pregnancies

What is a Chemical Pregnancy?
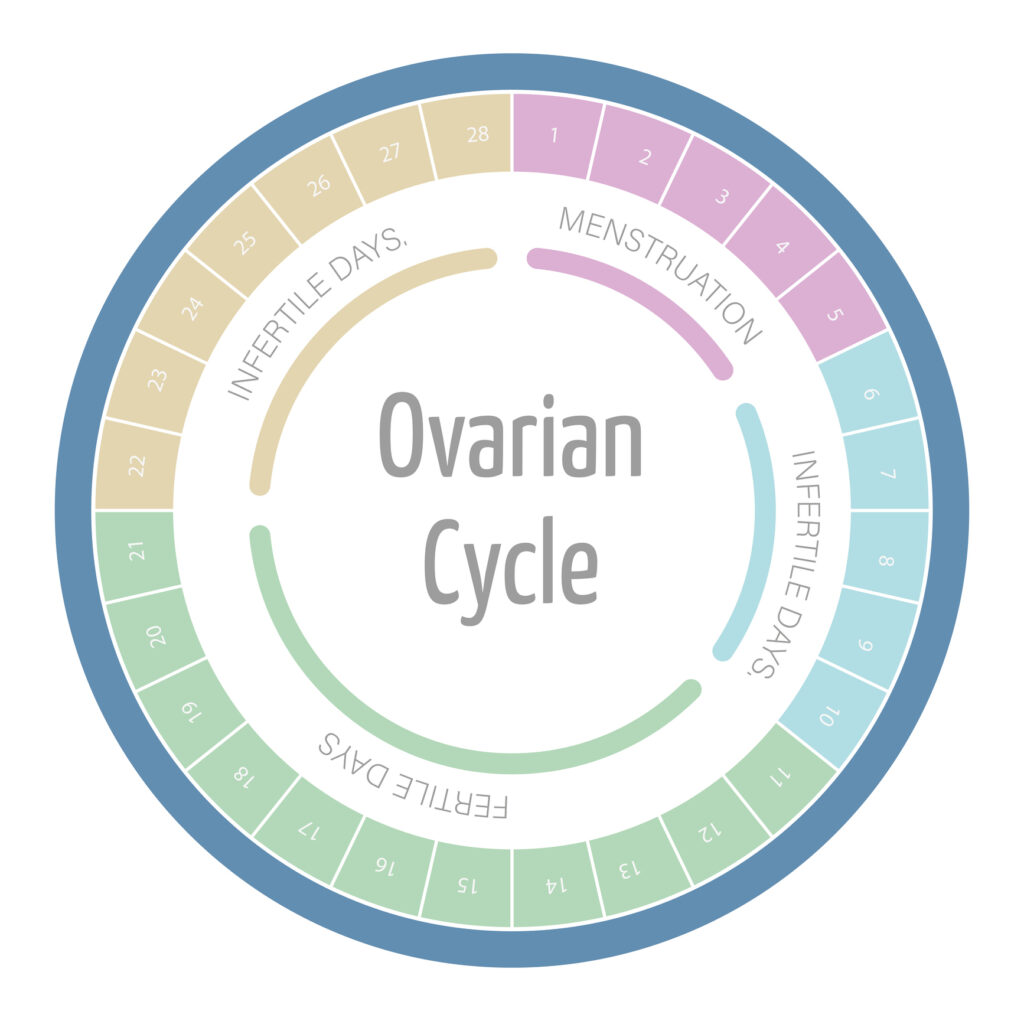
A chemical pregnancy, also known as an early miscarriage, occurs when a fertilized egg implants in the uterus but fails to develop past the early stages. It is called a “chemical pregnancy” due to the positive pregnancy test results that occur when the embryo implants and produces the hormone hCG (human chorionic gonadotropin). However, shortly after, the pregnancy is lost, often before it can be detected through ultrasound.
Chemical pregnancies are more common than many people realize, with estimates suggesting that up to 70% of conceptions may end in early pregnancy loss, many of which occur before a woman even realizes she is pregnant. While the emotional impact of a chemical pregnancy can be significant, it is essential to understand that they are usually due to biological factors beyond anyone’s control.
Causes and Symptoms of Chemical Pregnancies
The causes of chemical pregnancies are still not fully understood, but they are often attributed to chromosomal abnormalities in the embryo. Certain factors, such as hormonal imbalances, maternal age, and underlying medical conditions, may also contribute to the occurrence of chemical pregnancies.
It’s important to recognize that experiencing a chemical pregnancy does not indicate that there is an issue with future fertility. In most cases, it is a one-time occurrence and does not necessarily mean that there will be difficulties conceiving in the future. However, if recurrent chemical pregnancies become a concern, it may be advisable to seek guidance from a healthcare provider to explore potential underlying causes.
Symptoms of a chemical pregnancy are similar to those of an early miscarriage and may include vaginal bleeding, pelvic pain, and a sudden decrease in pregnancy symptoms. It is important to note that these symptoms can vary between individuals, and some women may not experience any noticeable signs of a chemical pregnancy.
Chemical Pregnancies and Fertility
The Impact of Chemical Pregnancies on Fertility
Experiencing a chemical pregnancy does not necessarily mean that a couple will have fertility issues in the future. In most cases, chemical pregnancies are isolated incidents that do not affect long-term fertility. However, recurrent chemical pregnancies may indicate underlying fertility problems and should be evaluated by a healthcare professional.
It is essential for individuals who have experienced a chemical pregnancy to seek emotional support during this challenging time. The emotional toll of pregnancy loss, no matter how early, can be significant. Counseling or support groups can provide a safe space to process feelings of grief, guilt, and disappointment.
Hormonal Changes After a Chemical Pregnancy
Following a chemical pregnancy, it is common for hormone levels, particularly hCG levels, to return to normal relatively quickly. This process may take a couple of weeks or longer, depending on the individual and the gestational age at which the pregnancy was lost. It is important to allow sufficient time for hormone levels to stabilize before attempting to conceive again.
In some cases, healthcare providers may recommend monitoring hormone levels post-chemical pregnancy to ensure that they return to baseline. This monitoring can help detect any potential complications or lingering hormonal imbalances that may require medical intervention. Open communication with a healthcare team is crucial during this time to address any concerns and ensure a healthy recovery.
The Science Behind Fertility Post Chemical Pregnancy
The Role of HCG Levels
HCG levels play a crucial role in early pregnancy. When a chemical pregnancy occurs, hCG levels may rise but then decline rapidly, indicating that the pregnancy was not viable. Monitoring hCG levels post-chemical pregnancy can help healthcare professionals assess the progress of hormone normalization and guide future fertility plans.
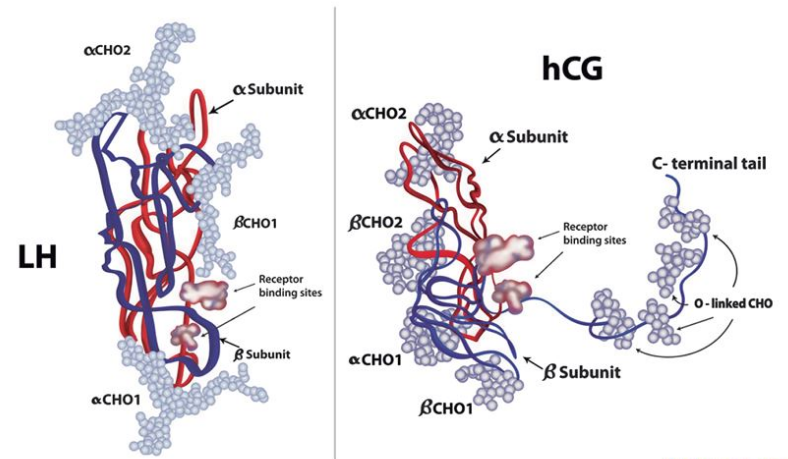
It is important to note that while hCG levels are a significant indicator of pregnancy, they are not the sole factor in determining fertility post-chemical pregnancy. Other hormonal changes and the overall health of the individual play crucial roles in the recovery process and subsequent fertility outcomes. Consulting with a healthcare provider can provide personalized guidance based on individual circumstances.
The Body’s Response to Early Pregnancy Loss
The body naturally undergoes a healing process following a chemical pregnancy. The uterine lining sheds, similar to a normal menstrual cycle. This process allows the body to prepare for future pregnancy attempts. However, it is essential to give the body time to recover fully before attempting to conceive again to ensure a healthy and successful pregnancy.
In addition to physical recovery, individuals may also experience emotional healing post-chemical pregnancy. Coping with the loss of a pregnancy, no matter how early, can be challenging. Seeking support from loved ones, counseling, or support groups can aid in the emotional healing process and help individuals navigate their fertility journey with resilience and hope.
Coping with Chemical Pregnancy
Emotional Impact of Chemical Pregnancy
Experiencing a chemical pregnancy can be emotionally challenging for both partners. It is common to feel grief, disappointment, and a sense of loss. It is crucial to give oneself permission to grieve and seek support from loved ones or professional counselors. Remember that emotional healing is just as important as physical healing.
During this difficult time, it’s important to acknowledge and validate the range of emotions you may be experiencing. From sadness and anger to confusion and guilt, each feeling is valid and part of the grieving process. It’s okay to not have all the answers or to feel overwhelmed by the rollercoaster of emotions. Taking the time to process these feelings can be a crucial step towards healing and moving forward.
Seeking Support After a Chemical Pregnancy
There are various resources available for individuals and couples seeking support after a chemical pregnancy. Support groups, online communities, and counseling services can provide a safe space to share experiences, gain coping strategies, and find solace in knowing that others have gone through similar journeys.
Connecting with others who have experienced a chemical pregnancy can offer a sense of community and understanding that may not be found elsewhere. Hearing stories of resilience and hope from those who have navigated similar challenges can be a source of comfort and strength. Additionally, seeking professional help from therapists or counselors trained in reproductive health can provide tailored support to address specific emotional needs and facilitate healing.
Prevention and Future Pregnancies
Can Chemical Pregnancies be Prevented?
While it is not always possible to prevent a chemical pregnancy, certain lifestyle choices and precautions may reduce the risk. Maintaining a healthy lifestyle, managing underlying medical conditions, and seeking prompt medical attention when any concerning symptoms arise can contribute to a healthier pregnancy outcome.
It is important to note that chemical pregnancies are often caused by chromosomal abnormalities in the fertilized egg, making them difficult to prevent through lifestyle changes alone. However, maintaining a balanced diet rich in essential nutrients like folic acid, avoiding harmful substances such as tobacco and excessive alcohol, and staying physically active can create a supportive environment for a potential pregnancy.
Planning for Future Pregnancies After a Chemical Pregnancy
After experiencing a chemical pregnancy, it is essential to allow time for physical and emotional healing before embarking on the journey of conception again. Consulting with a healthcare professional or a fertility specialist can help create a personalized plan to address any concerns and maximize the chances of a successful pregnancy in the future.
Furthermore, exploring alternative therapies such as acupuncture or mindfulness practices can aid in reducing stress levels and promoting overall well-being, which are crucial factors in preparing for a future pregnancy. It is also advisable to educate oneself about the various fertility treatments available, should they be needed, to increase the likelihood of a successful conception.
In summary, while chemical pregnancies may raise concerns about fertility, most individuals who experience them will go on to have successful pregnancies. Understanding the science behind chemical pregnancies, seeking support, and taking necessary precautions can help individuals navigate these challenging experiences, ultimately leading them closer to the dream of growing their family.