Letrozole for Fertility Treatment: Pros, Cons, Side Effects, and Patient Testimonials
Unlocking the Potential of Letrozole for Fertility Enhancement
Introduction
Fertility treatments have come a long way in recent years, providing hope and options for millions of couples worldwide. One of the latest advancements in this field is the use of Letrozole, a medication traditionally prescribed to treat breast cancer. This article will explore the benefits and drawbacks of Letrozole for fertility treatment, outline potential side effects, and provide firsthand patient testimonials to help you make an informed decision.
What is Letrozole?
Letrozole, sold under the brand name Femara, is an oral non-steroidal aromatase inhibitor. Originally developed for postmenopausal women with hormone receptor-positive breast cancer, it works by blocking the production of estrogen. In recent years, Letrozole has gained popularity as an off-label fertility treatment due to its ability to stimulate ovulation.
Pros of Letrozole for Fertility Treatment
- Effective for Ovulation Induction
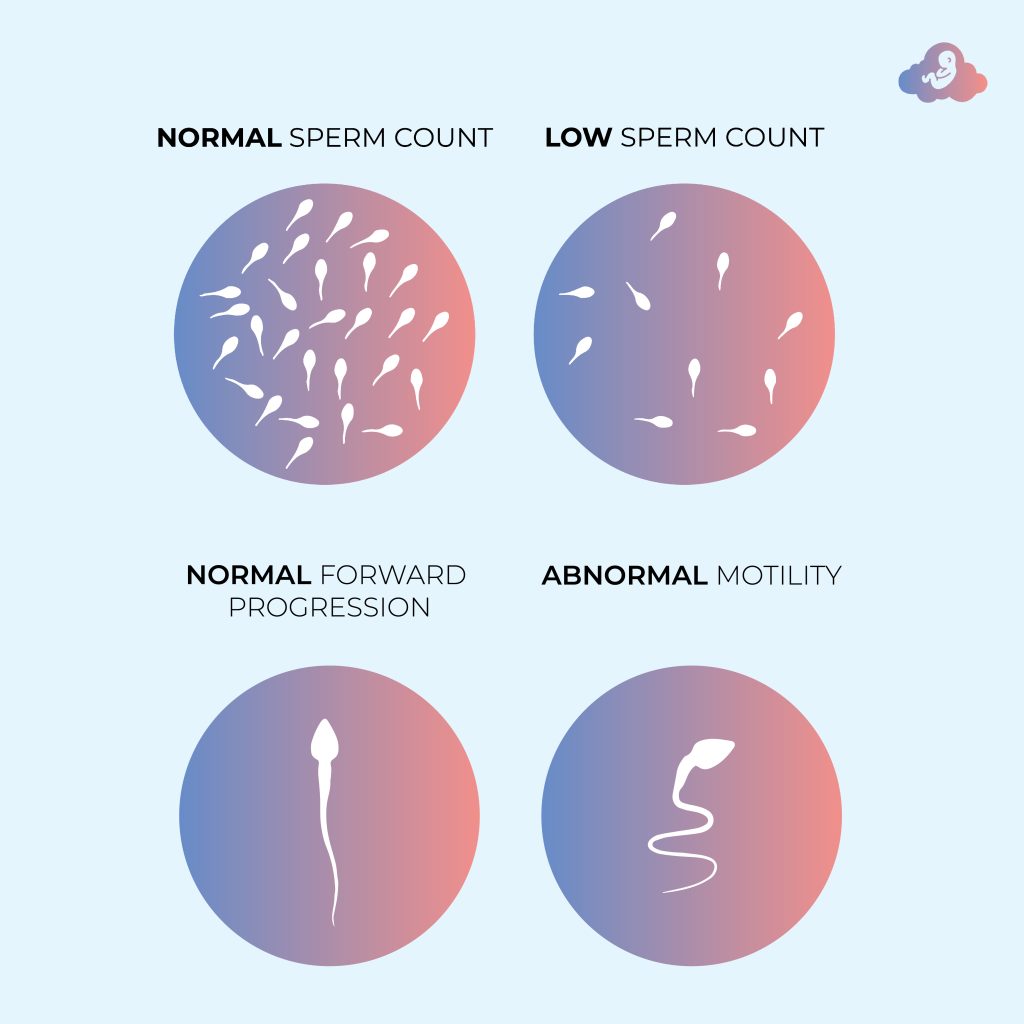
Letrozole has shown to be effective in inducing ovulation, particularly in women with Polycystic Ovary Syndrome (PCOS). It helps increase the production of follicle-stimulating hormone (FSH), which in turn promotes the growth of ovarian follicles and the release of eggs.
- Fewer Multiple Pregnancies
Compared to Clomiphene Citrate (Clomid), another popular fertility drug, Letrozole has a lower incidence of multiple pregnancies. This is an important consideration, as multiple pregnancies come with increased risks for both the mother and the babies.
- Minimal Interference with Endometrial Lining
Letrozole has a shorter half-life compared to Clomid, which means it is eliminated from the body more quickly. As a result, it has less impact on the endometrial lining, which is crucial for embryo implantation and the development of a healthy pregnancy.
- Lower Risk of Ovarian Hyperstimulation Syndrome (OHSS)
OHSS is a potentially life-threatening condition that can occur in women undergoing fertility treatments. Letrozole has a lower risk of causing OHSS compared to other fertility drugs, such as gonadotropins.
Cons of Letrozole for Fertility Treatment
- Off-Label Use
As mentioned earlier, Letrozole is not FDA-approved for fertility treatment. While many fertility specialists have successfully used it off-label, it is essential to discuss the implications and potential risks with your doctor.
- Limited Research on Long-term Effects
Although there is a growing body of evidence supporting the use of Letrozole for fertility treatment, there is still limited research on its long-term effects on both the mother and the child. Further studies are needed to fully understand the safety profile of this drug.
Possible Side Effects of Letrozole
Like any medication, Letrozole comes with potential side effects. Some of the most common side effects include:
- Hot flashes
- Headaches
- Dizziness
- Fatigue
- Breast tenderness
- Nausea
- Joint and muscle pain
- Mood swings
It is essential to monitor any side effects and discuss them with your healthcare provider. In some cases, the dosage of Letrozole may need to be adjusted to minimize adverse effects.
Patient Testimonials
To provide a well-rounded perspective, we have gathered testimonials from women who have used Letrozole for fertility treatment. These stories highlight both the successes and the challenges associated with this medication.
Testimonial 1 (Elizabeth G.): Success with Letrozole
“After years of trying to conceive, I was diagnosed with PCOS. My doctor suggested Letrozole, and I was hesitant at first, given it’s an off-label use. However, after discussing the potential benefits and risks, I decided to give it a try. To my amazement, I became pregnant after just two cycles! My pregnancy was healthy, and I now have a beautiful baby girl. I am so grateful for Letrozole and the chance it gave me to become a mother.”
Testimonial 2 (Shakiya J.): Side Effects and Persistence
“When I started taking Letrozole, I experienced some side effects like hot flashes and headaches. It was uncomfortable, but my doctor reassured me that these were common and would likely subside as my body adjusted to the medication. After three cycles, I still hadn’t conceived, but my doctor encouraged me to continue with the treatment. On my fifth cycle, I finally got a positive pregnancy test! Now, I have a healthy baby boy, and I’m thankful for my doctor’s encouragement and the effectiveness of Letrozole.”
Testimonial 3 (Meghan A.): Unsuccessful Experience
“Unfortunately, Letrozole didn’t work for me. I tried it for six cycles, and while I did ovulate, I never became pregnant. The side effects were also tough to deal with, especially the mood swings and fatigue. My doctor and I decided to explore other options, such as in-vitro fertilization (IVF), which eventually led to the birth of my daughter. While Letrozole didn’t work for me, I understand that every person is different, and it might work well for others.”
Conclusion
Letrozole offers a promising option for those struggling with fertility issues, particularly women with PCOS. Its effectiveness in inducing ovulation, lower risk of multiple pregnancies and OHSS, and minimal interference with endometrial lining make it an attractive choice. However, as with any medication, it is essential to weigh the pros and cons, be aware of potential side effects, and consult with your healthcare provider to determine if Letrozole is the right choice for your fertility journey.
Always consult with a professional.
As the patient testimonials demonstrate, Letrozole has been successful for many but may not be the right solution for everyone. Open communication with your doctor and persistence in exploring the best treatment options for your unique situation are vital in achieving your goal of parenthood.
What works for you?
While we work hard to bring you the most accurate and relevant information available on fertility, it’s important to remember that each person’s journey is unique. The guidance provided here is intended for general knowledge and may not directly apply to your situation. Fertility challenges should always be discussed with a licensed medical professional who can offer personalized advice tailored to your individual health history and needs. Beyond medical treatments, there are many ways to support your fertility naturally.
Reducing stress, maintaining a healthy diet, getting regular exercise, and ensuring adequate sleep can all play important roles in optimizing your fertility health. Simple changes such as managing stress through mindfulness, yoga, or meditation and prioritizing quality sleep can improve overall well-being and contribute to a more balanced approach to fertility. However, always consult a fertility specialist to get professional advice and recommendations suited to your personal circumstances. Your health and fertility are complex and unique, and professional guidance is essential to ensure you are on the right path for your body and your goals.
Fertility success starts with expert advice – don’t miss your chance, book a consultation today.