Discover the potential benefits and side effects of using Clomid 50mg for male fertility.
Clomid 50mg for Male: Benefits and Side Effects
In recent years, Clomid 50mg has gained popularity among males for its potential benefits in improving testosterone levels and fertility. However, it’s important to understand both the benefits and side effects before considering the use of this medication. Let’s delve deeper into what Clomid 50mg is, how it works, its potential benefits, and the possible side effects that males should be aware of. Additionally, we’ll explore some precautions and considerations to keep in mind when taking Clomid 50mg.
Understanding Clomid 50mg
What is Clomid 50mg?
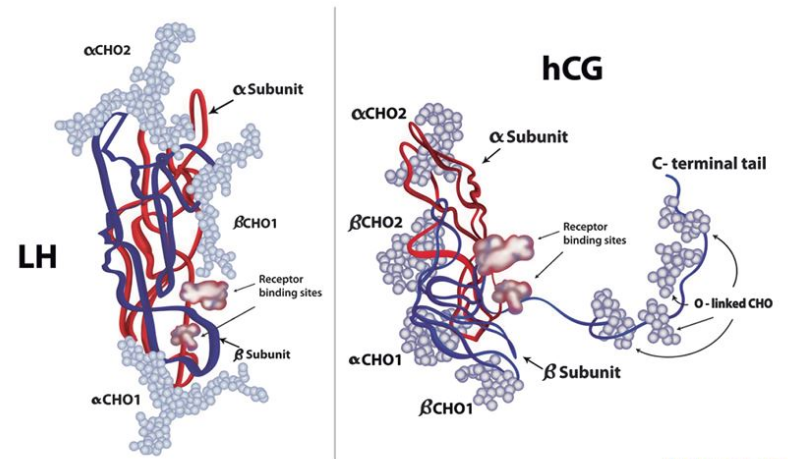
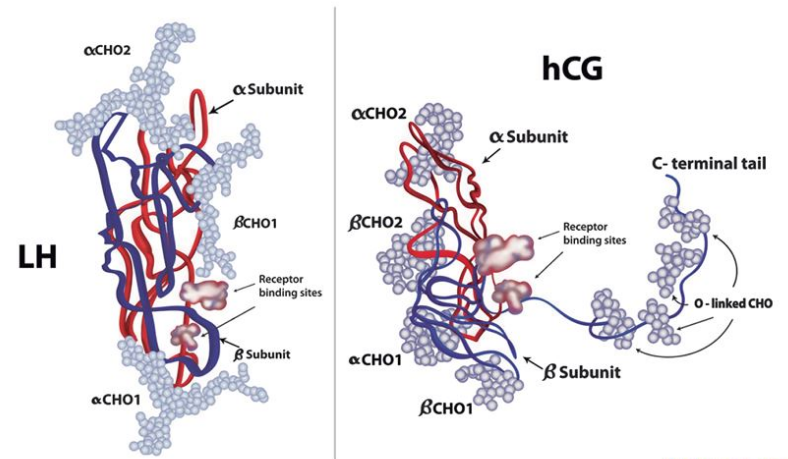
Clomid 50mg, or clomiphene citrate, is a medication commonly used in the field of reproductive medicine. Originally developed to treat female infertility, it works by stimulating the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH), both of which are essential for the production of testosterone in males.
Clomid 50mg is often prescribed to men with low testosterone levels, a condition known as hypogonadism. Low testosterone can lead to a variety of symptoms, including reduced libido, erectile dysfunction, fatigue, and decreased muscle mass. By boosting testosterone levels, Clomid 50mg can help alleviate these symptoms and improve overall quality of life.
How Does Clomid 50mg Work?
Clomid 50mg works by blocking estrogen receptors in the hypothalamus, a gland that regulates hormonal balance in the body. This leads to an increase in FSH and LH production, which in turn stimulates the testes to produce more testosterone. By enhancing the natural production of testosterone, Clomid 50mg can potentially address hormonal imbalances and improve fertility in males.
It is important to note that Clomid 50mg should only be taken under the supervision of a healthcare provider, as improper use can lead to potential side effects such as mood swings, hot flashes, and vision disturbances. Regular monitoring of hormone levels and overall health is crucial to ensure the safe and effective use of this medication.
The Benefits of Clomid 50mg for Males
Boosting Testosterone Levels
One of the primary benefits of Clomid 50mg for males is its ability to boost testosterone levels. Testosterone plays a crucial role in various bodily functions, including muscle development, bone density, and sexual function. By increasing testosterone production, Clomid 50mg may help alleviate symptoms of low testosterone such as fatigue, reduced libido, and mood disturbances.
Furthermore, the boost in testosterone levels provided by Clomid 50mg can also have positive effects on overall energy levels and cognitive function. Increased testosterone has been linked to improved focus, motivation, and mental clarity, which can be beneficial for individuals looking to enhance their daily productivity and overall well-being.
Improving Fertility
Another significant benefit of Clomid 50mg is its potential to improve fertility in males. By increasing the production of FSH and LH, Clomid 50mg stimulates the testes to produce more sperm. This can be particularly beneficial for men with low sperm count or poor sperm motility, as it may enhance their chances of achieving pregnancy.
In addition to improving sperm production, Clomid 50mg may also have a positive impact on the quality of sperm. Studies have shown that Clomid 50mg can help increase sperm motility and morphology, which are important factors for successful fertilization. This dual action on both sperm quantity and quality makes Clomid 50mg a valuable option for men looking to enhance their fertility.
Enhancing Athletic Performance
Some athletes and bodybuilders have started using Clomid 50mg as a performance-enhancing drug due to its ability to boost testosterone levels naturally. By increasing testosterone production, Clomid 50mg may help improve muscle strength, endurance, and overall athletic performance. However, it’s worth noting that the use of Clomid 50mg for athletic purposes is controversial and may be prohibited in certain sports organizations.
Moreover, the potential benefits of Clomid 50mg for athletic performance extend beyond just physical attributes. Improved testosterone levels can also lead to enhanced recovery times after strenuous workouts, allowing athletes to train more frequently and intensely. This accelerated recovery process can contribute to greater gains in muscle mass and overall fitness levels over time.
The Side Effects of Clomid 50mg in Males
Clomid 50mg, a medication commonly prescribed to treat infertility in women, is also sometimes used off-label in males to address hormonal imbalances. While Clomid 50mg has potential benefits in certain cases, it’s essential to be aware of the possible side effects that may accompany its use in men.
Physical Side Effects
Some males may experience physical side effects while taking Clomid 50mg. These can include hot flashes, headaches, blurred vision, or abdominal discomfort. It’s important to note that these side effects are typically temporary and tend to subside once the medication is discontinued. However, individuals should always consult their healthcare provider if they experience persistent or severe physical side effects.
Psychological Side Effects
In addition to physical side effects, Clomid 50mg can also lead to psychological symptoms in some male users. These may range from mood swings and irritability to more serious issues such as depression and anxiety. Monitoring and discussing any changes in mood or mental well-being with a healthcare provider is crucial while taking Clomid 50mg to ensure proper support and management of these potential side effects.
Long-term Side Effects
While studies on the long-term use of Clomid 50mg in males are currently limited, there is a theoretical concern regarding potential long-term side effects. Prolonged exposure to the medication may carry risks such as an increased likelihood of developing certain health conditions, including cardiovascular disorders or blood clotting abnormalities. Further research and clinical studies are necessary to fully understand the implications of extended Clomid 50mg use on male health and well-being.
Precautions and Considerations when Taking Clomid 50mg
Drug Interactions
If you’re considering taking Clomid 50mg, it’s crucial to inform your healthcare provider about any medications you’re currently taking. Certain drugs, such as aromatase inhibitors or testosterone replacement therapy, can interact with Clomid 50mg and potentially affect its effectiveness or increase the risk of side effects.
Health Conditions and Clomid 50mg
Individuals with certain medical conditions, such as liver disease, kidney disease, or hormone-related cancers, may be advised against taking Clomid 50mg. It’s essential to discuss your medical history with a healthcare provider to determine if Clomid 50mg is a suitable option for you.
Lifestyle Factors and Clomid 50mg Use
Lifestyle factors, such as smoking, excessive alcohol consumption, or obesity, can impact the effectiveness of Clomid 50mg. Maintaining a healthy lifestyle by following a balanced diet, exercising regularly, and managing stress can enhance the potential benefits of Clomid 50mg.
When it comes to drug interactions, it’s important to note that Clomid 50mg may also interact with certain herbal supplements or over-the-counter medications. It’s always best to disclose all the substances you are taking, including those that may seem harmless or insignificant. Your healthcare provider will be able to assess any potential interactions and make appropriate recommendations.
In addition to health conditions, it’s worth mentioning that age can also play a role in the suitability of Clomid 50mg. While it is commonly prescribed for men experiencing fertility issues, older individuals may have different responses to the medication. It’s important to have a thorough discussion with your healthcare provider about the potential benefits and risks based on your specific age and circumstances.
Furthermore, it’s essential to consider the duration of Clomid 50mg use. Long-term usage may have different implications compared to short-term use. Your healthcare provider will be able to guide you on the appropriate duration of treatment and any necessary monitoring that may be required.
In conclusion, Clomid 50mg can potentially offer benefits for males, including boosting testosterone levels, improving fertility, and enhancing athletic performance. However, it’s important to weigh these benefits against the possible side effects and consider the precautions and considerations outlined above. Before starting Clomid 50mg, it’s crucial to consult with a healthcare provider who can provide personalized advice and monitor your progress to ensure safe and effective usage.