Discover the incredible advantages of HCG testosterone therapy for men, including increased energy, improved muscle mass, and enhanced overall well-being.
The Benefits of HCG Testosterone for Men
In recent years, there has been a growing interest in the benefits of HCG testosterone for men. This hormone therapy has gained popularity for its potential to improve male health and well-being. Understanding HCG testosterone and its impact on the body is key to unlocking its benefits.
Understanding HCG Testosterone
What is HCG Testosterone?
HCG, short for human chorionic gonadotropin, is a hormone produced naturally in the human body. It is primarily associated with pregnancy, as it is responsible for maintaining the production of other vital hormones during this time. However, HCG also plays a role in male health, particularly in relation to testosterone.
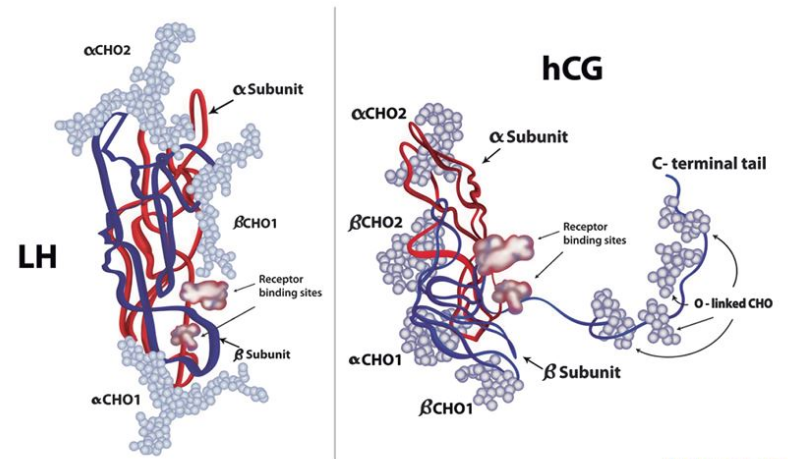
When it comes to male health, testosterone is often referred to as the primary male sex hormone. It is responsible for the development of male reproductive tissues, such as the testes and prostate, as well as promoting secondary sexual characteristics like increased muscle mass and body hair. Testosterone levels naturally decline with age, leading to symptoms such as decreased libido, fatigue, and reduced muscle mass.
How Does HCG Testosterone Work in the Body?
HCG testosterone therapy involves injecting the HCG hormone into the body. This stimulates the production of testosterone in the testes. Testosterone is a crucial hormone for men, responsible for maintaining sexual function, muscle growth, and bone density. By increasing testosterone levels, HCG therapy aims to improve overall male health.
It’s important to note that HCG therapy should only be administered under the supervision of a healthcare provider, as improper use can lead to potential side effects. Monitoring hormone levels and adjusting dosage accordingly is crucial to ensure the effectiveness and safety of HCG testosterone therapy.
The Role of HCG Testosterone in Men’s Health
When delving into the realm of men’s health, the significance of HCG testosterone therapy cannot be overstated. This specialized treatment plays a crucial role in addressing various health concerns that stem from low testosterone levels in men. From fertility issues to muscle development, HCG testosterone therapy offers a multifaceted approach to enhancing overall well-being.
HCG Testosterone and Male Fertility
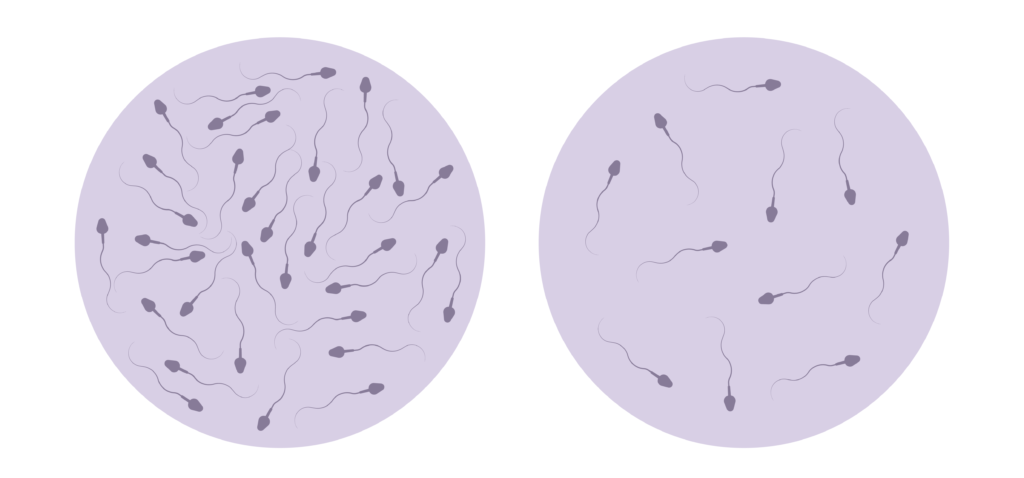
Male fertility is a complex and delicate aspect of reproductive health that can be influenced by testosterone levels. Low testosterone levels have been linked to reduced sperm production and fertility challenges in men. Through the administration of HCG testosterone therapy, individuals may witness a notable improvement in sperm count and quality. This enhancement not only holds the potential to elevate fertility levels but also to increase the likelihood of successful conception, providing hope and optimism for individuals and couples facing such concerns.
HCG Testosterone and Muscle Development
Another compelling facet of HCG testosterone therapy lies in its impact on muscle development. Testosterone serves as a primary driver of muscle growth and strength in the male body. When testosterone levels are suboptimal, individuals may experience a decline in muscle mass and overall physical performance. By leveraging HCG testosterone therapy to elevate testosterone levels, men can potentially witness significant advancements in muscle development. Whether the goal is to cultivate lean muscle mass or enhance athletic prowess, the benefits of this therapy extend beyond mere physical appearance, delving into the realm of functional fitness and overall well-being.
The Health Benefits of HCG Testosterone
When it comes to boosting energy levels, HCG testosterone therapy can be a game-changer. Low testosterone levels can contribute to feelings of fatigue and decreased energy levels, affecting daily activities and overall quality of life. By undergoing HCG testosterone therapy, individuals can experience a significant increase in energy levels and combat fatigue effectively. This boost in energy not only enhances physical performance but also improves mental clarity and overall well-being.
Moreover, HCG testosterone therapy offers benefits beyond just energy levels. Testosterone plays a crucial role in the regulation of body fat and metabolism. Low testosterone levels can lead to an increase in body fat and make it challenging to lose weight. By undergoing HCG testosterone therapy, individuals can optimize their testosterone levels, potentially aiding in weight loss and management. When combined with a balanced diet and regular exercise, HCG therapy can provide additional support in achieving weight management goals, leading to a healthier and more active lifestyle.
Boosting Energy Levels with HCG Testosterone
Low testosterone levels can contribute to feelings of fatigue and decreased energy levels. HCG testosterone therapy has been shown to increase energy and combat fatigue, leading to improved overall well-being and quality of life.
HCG Testosterone and Weight Management
Testosterone plays a role in the regulation of body fat and metabolism. Low testosterone levels can lead to increased body fat and difficulty in losing weight. HCG testosterone therapy can help optimize testosterone levels, potentially aiding in weight loss and management. Combined with a healthy diet and exercise, HCG therapy may offer additional support in achieving weight management goals.
Potential Side Effects of HCG Testosterone
Common Side Effects of HCG Testosterone
While HCG testosterone therapy is generally safe and well-tolerated, there are some potential side effects to be aware of. These can include acne, mood swings, fluid retention, and changes in libido. It is important to discuss any concerns or potential side effects with a healthcare provider to ensure the best possible outcomes.
Acne, one of the common side effects of HCG testosterone therapy, can be managed with proper skincare routines and, in some cases, medication. Mood swings, another potential side effect, may vary in intensity and duration from person to person. Fluid retention, while usually temporary, can be uncomfortable and may require adjustments to the treatment plan. Changes in libido are also possible, but often stabilize as the body adapts to the therapy.
Managing Side Effects and Risks
If side effects occur, they are often mild and tend to subside as the body adjusts to therapy. However, it is important to work closely with a healthcare provider to monitor hormone levels and manage any potential risks. Regular check-ups and open communication can help ensure the safe and effective use of HCG testosterone therapy.
Monitoring hormone levels through blood tests is a crucial aspect of managing side effects and risks associated with HCG testosterone therapy. These tests help healthcare providers track the impact of the treatment on the body and make informed decisions about any necessary adjustments. Additionally, maintaining a healthy lifestyle, including regular exercise and a balanced diet, can support the body’s response to therapy and minimize potential side effects. Adequate hydration and sufficient rest are also important factors in promoting overall well-being during HCG testosterone treatment.
The Process of HCG Testosterone Therapy
Preparing for HCG Testosterone Therapy
Prior to starting HCG testosterone therapy, a comprehensive medical evaluation is typically conducted. This includes assessing hormone levels, overall health, and discussing any potential risks or concerns. Based on the assessment, a personalized treatment plan can be developed to address individual needs and goals.
During the initial evaluation for HCG testosterone therapy, healthcare providers may also discuss lifestyle factors that can impact treatment outcomes. Factors such as diet, exercise, stress levels, and sleep patterns can all play a role in hormone balance and overall well-being. Making positive changes in these areas can complement the effects of therapy and optimize results.
What to Expect During HCG Testosterone Therapy
HCG testosterone therapy typically involves regular injections of HCG hormone, as prescribed by a healthcare provider. Routine monitoring of hormone levels and follow-up visits are necessary to track progress and make any necessary adjustments to the treatment plan. It is important to communicate openly with a healthcare provider throughout the therapy to ensure the best possible outcomes.
Aside from injections, individuals undergoing HCG testosterone therapy may also be advised to make specific dietary or lifestyle changes to support the treatment. These changes could include increasing protein intake, incorporating strength training exercises, and managing stress levels. By taking a holistic approach to health, individuals can enhance the benefits of therapy and promote long-term well-being.
In conclusion, HCG testosterone therapy has shown promising benefits for men’s health. By increasing testosterone levels, this therapy can potentially improve fertility, muscle development, energy levels, weight management, and overall well-being. While there are potential side effects and risks to consider, working closely with healthcare professionals can help ensure the safe and effective use of HCG testosterone therapy. If you are interested in exploring HCG testosterone therapy, consulting with a healthcare provider is recommended to determine if it is a suitable option for you.